My Past and Future at U of T: Helena Lan’s Perspective
Hey everyone, it’s been a while since I posted here. In case you don’t remember me – my name is Helena Lan, and I started in Professor Pascal Tyrrell’s group as a ROP299 student. Fast forward to the present, I have finished my specialist program in pharmacology, and will be graduating with an Honours Bachelor of Science degree later this month! But if you think that I am finally leaving U of T – nope, my journey is not over yet. This August, I will be living my dream of many years as I start my MD training at U of T! As I prepare to begin the next chapter of my life, I wanted to share with you how my involvement in Prof. Tyrrell’s group paved the way for me achieving my goal today.
Afterwards, I continued on as a research assistant, where I explored the need for statistics and research methodology training in the medical imaging department. My early research endeavours showed me that research was not just pipetting; there is a diversity of research that can drive innovations and improve patient care.
Walk Like an Egyptian!
So, in my last post I talked a little about Mesopotamian medicine (see here). I am certain many of you were thinking: “What? Should he not be talking about ancient Egypt?”. Well, of course, you are right – kind of…
 Egypt rose under the pharaohs during the same period as the Mesopotamian kingdoms (from about 3000 BC). They were known for their crazy ambition and technological prowess. Their medicine was very similar to that of the Mesopotamians in that it was influenced strongly by superstition and religious beliefs. They too had three types of healers: the swnu who practiced medicine, and, of course, the priests and the sorcerers…
Egypt rose under the pharaohs during the same period as the Mesopotamian kingdoms (from about 3000 BC). They were known for their crazy ambition and technological prowess. Their medicine was very similar to that of the Mesopotamians in that it was influenced strongly by superstition and religious beliefs. They too had three types of healers: the swnu who practiced medicine, and, of course, the priests and the sorcerers…
One of the reasons that ancient Egyptian medicine had a greater influence on modern medicine was that they were very good at documenting and archiving their work. The Ebers papyrus (c. 1550 BC) was their principal medical document that measured over 20 meters long (it is a scroll after all) and is the oldest surviving medical book.
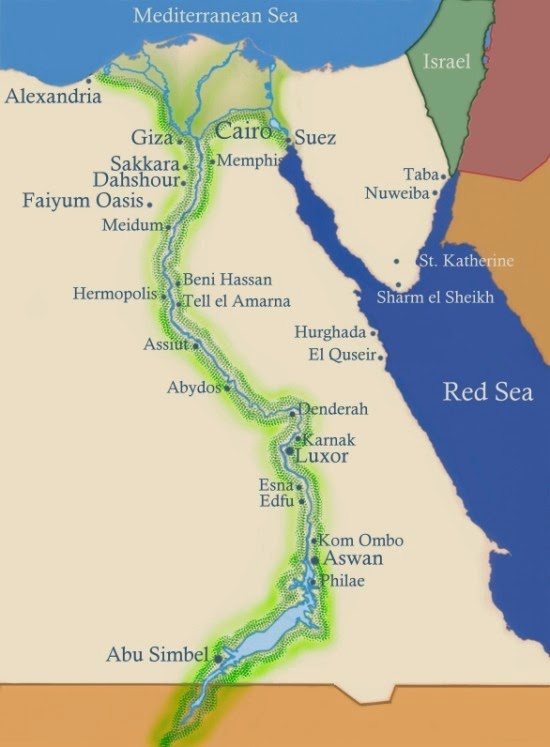 The Egyptians believed we were all born healthy but were susceptible to disorders caused by demons or by intestinal putrefaction. So the importance of eating your fruits and veggies was started way long ago! They also compared our vascular network to that of the River Nile and its canals and, therefore, it was important to keep the flow free from obstructions (see here for another interesting comparison!). Though they did not appreciate vascular plaques (atheroma) at the time they had already started to figure out the importance of a healthy vasculature. Cool!
The Egyptians believed we were all born healthy but were susceptible to disorders caused by demons or by intestinal putrefaction. So the importance of eating your fruits and veggies was started way long ago! They also compared our vascular network to that of the River Nile and its canals and, therefore, it was important to keep the flow free from obstructions (see here for another interesting comparison!). Though they did not appreciate vascular plaques (atheroma) at the time they had already started to figure out the importance of a healthy vasculature. Cool!
As with Mesopotamia, Egypt’s powerful governance created a good environment for organized medical practice. However, because both regimes were highly codified (implying many strict rules based on religion and superstition that did not allow for discussion and experimentation) it will not be until ancient Greece that the roots of modern medicine will take hold.
Dance around your living room (in private if you must) to Walk Like an Egyptian by The Bangles in order to decompress and…
… I’ll see you in the blogosphere.
Pascal Tyrrell
Who is Going to the Karolinska Institute this Summer? Helena Lan Is, That’s Who!!!!

The Karolinska Institutet is one of the world’s leading medical universities and is located in Stockholm, Sweden. Did you know that in 1895 Alfred Nobel appointed the Karolinska Institutet to annually award the Nobel Prize in medicine or physiology? Now you do.
So, you may have read my previous post about “Connectory”. Well today I want to talk to you about one of my Research Opportunity Program students at the University of Toronto, Helena Lan. Not only was she a star student with me last summer (see her timeline post here) but she has continued on with our MiVIP group contributing to a systematic review on research methodology and biostatistics in medical imaging (stop rolling your eyes, it IS an interesting topic!).
Well she just found out that that she has been invited to work at the Karolinska Institute this summer as part of the Summer Research Abroad Program at the University of Toronto which is sponsored by the the Centre for International Experience. WOW!!!
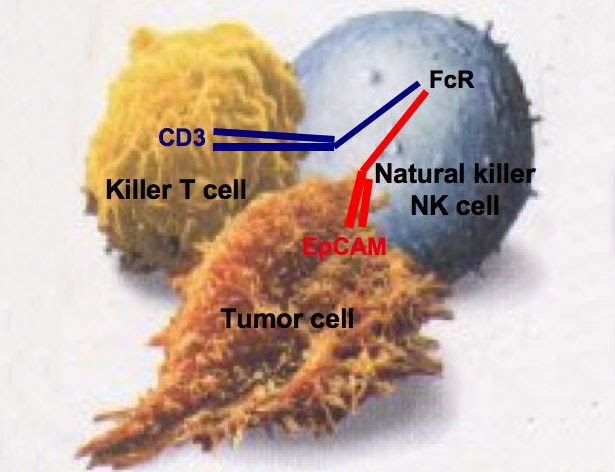
Her supervisor will be Dr. Sofia Johansson, an assistant professor at Karolinska Institutet. Her research is focused on natural killer cell biology. You can find her research interests here.
Want to know about what natural killer cells do as part of our innate immune system? Watch this cool video.
Cool right? Well, I enjoyed it anyway. Maybe you need to watch Mr Brightside by The Killers to recover and…
… I’ll see you in the blogosphere.
PS: Congratulations Helena!!!
Pascal Tyrrell
The story behind Connectory…
So, you are reading our blog thinking Pascal is a nut – that much is clear – but what of all the students plugged into his group? Are they nuts too?
 Well maybe, but today I am going to talk to you about the group of four (not the group of seven) who started small and grew to be Connectory. John, Maria, Natasha, and Roger met in a graduate course at the University of Toronto and decided to work together on a project about innovation. That’s when they met me, joined “the program”, and got busy! Starting any endeavour from scratch is no easy task. All four had never met before, all came from very different academic backgrounds, and though their initial project was for “credit” the rest was on their own time.
Well maybe, but today I am going to talk to you about the group of four (not the group of seven) who started small and grew to be Connectory. John, Maria, Natasha, and Roger met in a graduate course at the University of Toronto and decided to work together on a project about innovation. That’s when they met me, joined “the program”, and got busy! Starting any endeavour from scratch is no easy task. All four had never met before, all came from very different academic backgrounds, and though their initial project was for “credit” the rest was on their own time.
There were some rough times at first but with perseverance comes success and Connectory was born and is just finishing up its first project as a new start-up business. Wow!
Essentially Connectory is a data management solutions software development consulting group that operates in the healthcare space. Check out their webpage here.
Ok, so what? Well this post is not only to congratulate these four on a job well done but also to encourage you to do the same. One thing is for sure: if you don’t try you will not succeed – ever. My programs are all about learning, trying new stuff, benefiting from your successes as well as your failures, and wait for it… giving back. Yup as Uncle Ben said in Spiderman: “With great power comes great responsibility“.
Just wanted to share a good story from our group with you today.
Listen to Bulletproof by La Roux to get pumped and…
… I’ll see you in the blogosphere!
Pascal Tyrrell
MiWord of the Day Is… Cinemaradiology!
Yes, it is Halloween today and my kids could barely contain themselves getting ready for school. I suspect today will not be very productive as they count down the minutes before heading out to terrorize my neighbors.
Anyway, how about this for a scary thought: cinemaradiology! In the late 1800’s John MacIntyre at the Gasgow Royal Infirmary experimented with producing X-ray motion pictures. What!!!? He tried exposing film by passing it between the screen of the fluoroscope and the x-ray tube and by simply filming the fluoroscopic screen. This latter method was very difficult because, as all of you budding radiologists know, the images viewed on the fluoroscope screen were dim and of poor resolution at the time.
For years researchers worked on perfecting cinemaradiology. However, during those early years of discovery they lost interest when they realized that sharper images were possible when BOTH patients and investigators were exposed together AND that excessive radiation was a bad thing – duh!
It would only be many many years later that fluoroscope screen technology would be improved to allow for brighter and higher resolution images (and without frying the patient and everyone around!).
To my knowledge, no actors from the cinemaradiology era ever became successful stars in Hollywood…
No need to use the MiWord of the day in a sentence today (see rules here) as I realize you are busy getting ready for Halloween and need a break!
Decompress listening to the classic song Thriller by the King of Pop Michael Jackson and I’ll see you in the blogosphere…
Pascal Tyrrell
MiWord of the Day Is… Cuckoo!
One of my favorite more serious films is One Flew Over the Cuckoo’s Nest. What does Jack Nicholson’s portrayal of a bad guy hoping for easy served time in a mental institution have to do with medical imaging? Well it all starts with the lobotomy. Not to spoil the story, suffice it to say that the movie broaches the topic of lobotomies and how ridiculous they were. Lobotomy was a form of neurosurgery that involved damaging the prefrontal cortex in order to “calm” certain mentally ill patients. Needless to say the procedure was controversial from the beginning (1935 to the early 1970’s) but the author of the discovery, Egas Moniz, was awarded the Nobel Prize in 1949. Maybe not the most sound of decisions by the committee. However, for the time, it was considered progress in a very challenging area of medicine – mental illness.
OK, medical imaging? Well as it turns out Moniz (do not confuse with St-Moriz, ahhh skiing…) is also known for developing cerebral angiography – a technique allowing the visualization of blood vessels in and around the brain.
Moniz was interested in finding a non-toxic substance that would be eliminated from the body, but would not be diluted by the flow of blood before the x-ray could be taken. Another requirement is that the substance could not cause an emboli or clot as this would be a bad thing. Moniz played with salts of iodine and bromine and settled on iodine because of its greater radiographic density. And voila, birth of iodinated radiocontrast agents still in use today. Cool.
Supposedly it took him 9 patients to perfect his angiogram technique. Don’t ask about the first 8…
Moral of the story is: lobotomy bad and cerebral angiography good.
Now for the fun part (see the rules here), using Cuckoo in a sentence by the end of the day:
Less serious: Someone won a Nobel Prize for developing the lobotomy? Are you cuckoo?
MiWord of the Day Is… Fluoroscope!
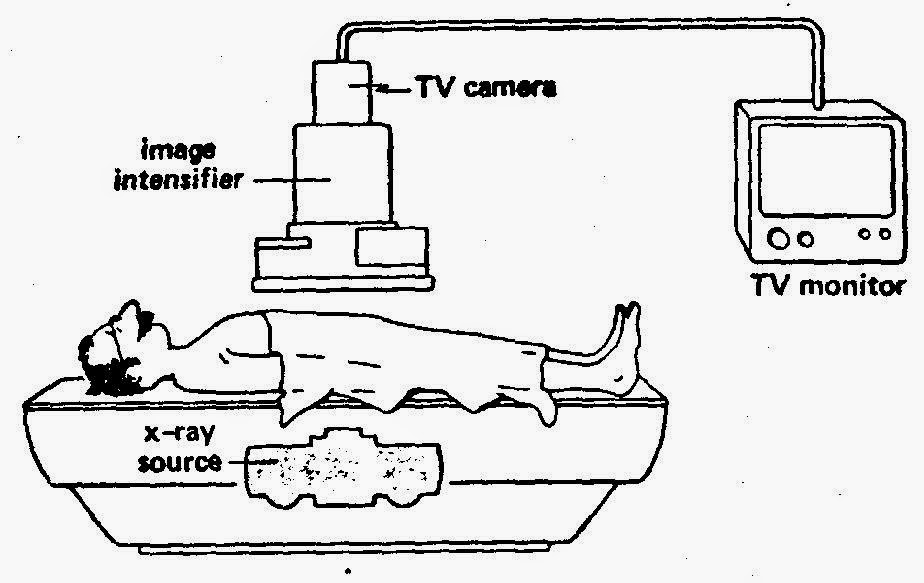
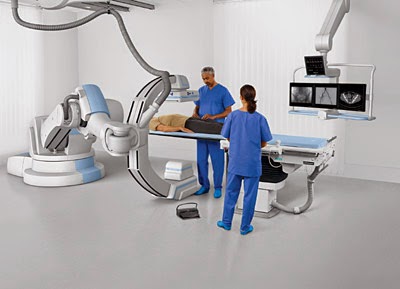 Fluoroscopes have come a long way over the years and are still used today in areas such as orthopedic surgery, gastrointestinal investigations, and angiography but, of course, the dose of x-rays a patient receives is minimized and closely monitored. Have a look at this machine from Siemen’s. “Beam me up Scotty!”.
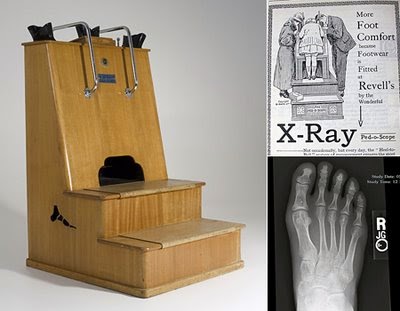
Fluoroscopes have come a long way over the years and are still used today in areas such as orthopedic surgery, gastrointestinal investigations, and angiography but, of course, the dose of x-rays a patient receives is minimized and closely monitored. Have a look at this machine from Siemen’s. “Beam me up Scotty!”.  Due to the enormous supply of portable x-ray machines at the time following the end of the war, Dr Jacob Lowe introduced the idea of using a modified portable x-ray machine in the shoe retail industry. Voila, fried feet fricassee for the next 50 years!
Due to the enormous supply of portable x-ray machines at the time following the end of the war, Dr Jacob Lowe introduced the idea of using a modified portable x-ray machine in the shoe retail industry. Voila, fried feet fricassee for the next 50 years!Now If were to be interested in using a fluoroscope to look at my feet I may be inclined to use a suit like this gentleman below is sporting…
 |
| WW I x-ray protection suit |
Now for the fun part, using Fluoroscope in a sentence by the end of the day:
Serious: Bob, did you know that the foot-o-scope was a modified fluoroscope used to view ones feet when fitting new shoes which delivered on average 13 Roentgens for every 20 second exposure?
Less serious: I heard grampa grumbling he can never find shoes that fit right anymore since they banned fluoroscopes in shoe stores. What is a fluoroscope mommy?
Listen to High Heels to decompress and I’ll see you in the blogosphere.
Pascal Tyrrell
MiWord of the Day Is… Radio!
Easy one today! I thought I would give everyone a break as you have all been working very hard on the MiWord of the day in the past weeks.
So, what does radio have to do with medical imaging? What a great question! The origin of the root word “Radio” is radiant energy. The radio you immediately think of is the one that is attached to your ear most of the time and has a DJ who selects music to play for your entertainment – along with ads to pay for the station’s bills! The use of “radio” to describe this form of wireless communication comes from the word radiotelegraphy.
How about if we were simply interested in a medical picture produced by radiant energy? Well you would end up with a radiograph AKA an x-ray! We talked about that word here. Do you see the trend? How about a picture produced by radiant energy in the visible light range of the electromagnetic spectrum? A photograph. Cool.
OK now suppose you are an MD working in the emergency department and someone presents with a lung disorder. What do you do? Generally, you order a chest radiograph. As you zap your patient with x-rays you expect that most of them will pass through the chest area – that is mostly filled with air – unchecked and will proceed to expose the film (or trigger the detector) resulting in a dark area. However, if the lungs become filled with abnormal substances more of the x-rays are blocked and result in a lighter (whiter) radiograph. What would you be looking for?

1- Pus – a combination of bacteria and white blood cells as seen with pneumonia.
2- Edema – fluid that leaks into the lungs as seen with heart failure.
3- Hemorrhage – bleeding into the lung cavity as seen with trauma.
4- a solid mass – as seen in lung cancer.
Today, we have to use “Radio” in a sentence (see rules here). Easy! Here are two examples to help you along:
Serious: Bob, you will need to remove your radio from your person before entering the MRI. No metal objects are permissible in the room.
Less serious: I went for a radiograph today and all they did was have me stand in a room by myself and that was it! What a relief. I thought for a moment I was scheduled for a radio-graft…!
Have a listen to my favorite Radiohead to decompress and…
… I’ll see you in the blogosphere,
Pascal Tyrrell
MiWord of the Day Is… Ionizing!
So what the heck is ionizing radiation? Well consider the following conundrum about x-rays. They can:
1- cause cancer
2- be used to detect cancer.
3- be used to treat cancer.
Whaaat? How does that work? We use the term ionizing when the radiation has sufficient energy to detach electrons from molecules causing them to become chemically reactive ions.
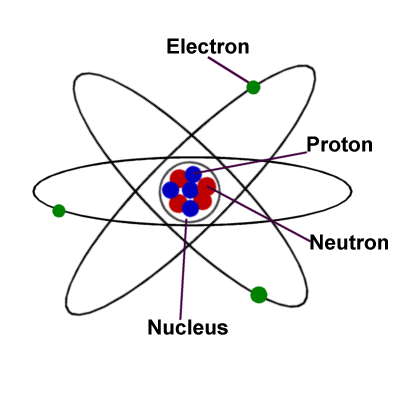
The name atom means “indivisable” and are incredibly small. They are made up of protons, neutrons, and electrons with about 99.9% of its mass concentrated in the nucleus that holds a positive charge. A surrounding negatively charged cloud of electrons makes up the difference and the atom stays together due to the attraction between the two.
OK, so here is the rub: if an atom gains or loses an electron it becomes an ion and generally results in a very chemically reactive substance. This process to produce an ion can be achieved by many ways but one of the most important is electromagnetic radiation (we’ve talked about this already here). Radioactive materials such as radium emit ionizing radiation as does x-ray tubes. There is even such a thing as cosmic radiation (Yup, we talked about that here!).
Now x-rays produce photons which are the same particles that make up visible light but at a much shorter wavelength and higher energy. When they penetrate through a solid object they will most often simply pass through. However, if they pass by close enough to an electron they can transfer their energy and in the process knock it out orbit producing an ion. Also, the more dense the object the more often the photons are blocked from travelling through resulting in a differential effect on a film or sensor placed on the opposite side. This is how we are able to see inside the body using x-rays.
The problem about ionizing radiation is that the resulting chemically reactive ions can result in DNA damage. Often the cell can repair itself resulting in no permanent damage. Other times, however, permanent damage occurs and can result in cell death (a good thing if they are cancerous cells) or DNA mutations that can in turn lead to the promotion of cancer – bummer.
Now on to using ionizing in a sentence today (not sure about the rules? See here):
Serious example – Bob, don’t stand too close to the x-ray machine. You wouldn’t want to be exposed to ionizing radiation that could damage the DNA in your cells…
Less serious – You wouldn’t believe what happened to me at work today! I was at the photocopy machine getting ready to change the toner cartridge and Bill from sales said:”Let me do that for you, Honey”. He is so ionizing or patronizing or whatever. He makes me mad…
Listen to Just Because by Raygun to get ready for the weekend and I’ll see you back in the blogosphere soon.
Pascal Tyrrell